Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124

BBC News, Johannesburg
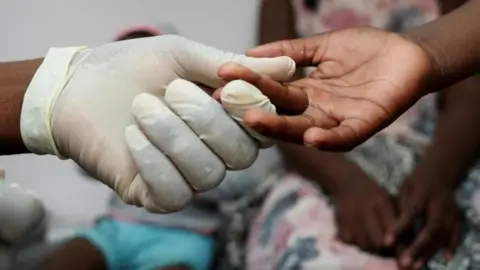 Reuters
ReutersGugu used his antiretrovirus from a clinic funded by USAID in central Johannesburg.
But when President Trump’s abbreviations to support funding were announced earlier this year, she and thousands of other HIV-positive patients in South Africa suddenly confronted the uncertain future.
Gugu was lucky, the clinic, where she received medicines that help suppress her symptoms, contacted her before closing.
“I was one of the people who managed to get their bulk medicines. I usually collect a three -month recipe. But before my clinic closed, they gave me medication for nine months.”
In September, it will exhaust the antiretrovs (ARVS), and then plans to go to its local public hospital for more.
A former sex worker, the 54-year-old realized that he was HIV-positive after leaving the industry.
Ten years ago, she received her breast cough and initially thought it was tuberculosis. She went to a doctor who told her she had breast infection and treats her for it.
But when treatment failed, she went to a clinic to get a HIV test.
“Until then, I already assumed that I was HIV-positive and told the nurse that.”
She has been right and has been on ARVS ever since. We do not use her real name at her request.
She is currently working as a coordinator of the NGO project.
“We help pregnant sex workers get their ARV to ensure that their children are born HIV negative. We also make home visits to make sure that mothers take their medicines on time and take care of their babies when they go to their monthly examinations.”
Many HIV-positive sexual workers in South Africa relied on private clinics funded by the already non-existent US, USAID assistance agency to obtain their prescriptions and treatments.
But most of the facilities closed after US President Donald Trump reduced most foreign help earlier this year.
Gugu believes that many sexual workers can be discouraged to go to public hospitals for their ARV if they can no longer receive them from clinics.
“The problem of going to public hospitals is the time factor. In order to serve these facilities, you have to arrive at 4 or 5am and they can spend the whole day waiting for their medicines. For sexual workers, time is money,” Gugu says.
She adds that she recently went to her local hospital with some friends to register her data and build a connection with the staff.
“The sister who attended us was very rough. She told us that there was nothing special about sexual workers.”
She believes that this can lead to many sexual workers do not undergo their medication, “especially because their hospital files contain a lot of personal information and the anxiety is that sometimes nurses in these local clinics are not always the most sensitive to working with this type of information.”
 Ghetto images
Ghetto imagesIn a report published on Thursday, the UN body responsible for the fight against HIV/AIDS does not separate the United States, but says the drastic cuts of a number of donors have sent shock waves around the world that that “phenomenal progress” in dealing with the disease risks being turnedS
“The new HIV infections have been reduced by 40% since 2010 and 4.4 million children have been protected from HIV’s acquisition since 2000. More than 26 million lives have been saved,” UNAIDS says, warning that if the world is not working, there can be an additional six million new HIV infections and four million AIDS related to 2029.
UNAIDS said that before financing the financing, the annual number of new HIV and death infections associated with AIDS have sunk to our lowest levels in more than 30 years.
All data published in the report are from before the US and other donors to reduce funding earlier this year. But it emphasizes how much progress can be lost as a result of these cuts.
Sub -Saharan Africa decreased in 56% in the number of new infections. The area is still the epicenter of the epidemic – half of all new infections last year were from the continent. But four African countries – Lesoto, Malawi, Rwanda and Zimbabwe – were on the road to achieve a 90% decrease in new infections by 2030 compared to 2010.
Another history of Africa’s success is the presentation of antiretrovirals, which help to suppress the symptoms of HIV. Among other medical progress in this area, they helped to increase life in Africa of Subsahara from 56 years in 2010 to 62 years in 2024.
The conversion began when the then US President George B Bush launched an ambitious HIV/AIDS program in 2003, stating that he would serve the “strategic and moral interests” of the United States.
Known as the President’s Emergency Plan for AIDS relief (PEPFAR), it has led to an investment of more than $ 100 billion ($ 74 billion) in the global response of HIV/AIDS – the most engagement of any nation to deal with a disease in the world.
South Africa has about 7.7 million people living with HIV, the largest number in the world, According to UnaidsS
About 5.9 million of them receive antiretroviral treatment, leading to a 66% reduction in AIDS -related deaths since 2010, the UN agency added.
The South Africa government says Pepfar funding has contributed about 17% to its HIV/AIDS program. The money has been used for various projects, including mobile clinics management to make it easier for patients to treat.
Reducing the Trump administration has caused concern that the infection percentage can jump again.
“I think we will begin to observe an increase in the number of HIV infections, the number of cases of tuberculosis, the number of other infectious diseases,” says Prof. Lynn Morris, Vice-Cantzer at the University of Johannesburg, “BBC told.
“And we will begin to see the conversion of what was essentially a true story of success. We came to some of these things.”
Gugu points out that treatment is a matter of life and death, especially for a vulnerable population as sexual workers.
“People do not want to default on their ARV. They are scared that they will die if they do not have access to them.
Cutting also affects studies aimed at finding a HIV vaccine and a cure for AIDS.
“There is a long -term impact, which is that we will not get new HIV vaccines,” added Prof. Morris.
“We will not hold on top of the viruses that spread.
South Africa was one of the world leaders in HIV’s research. Many of the drugs that help prevent the virus and have benefited from people around the world have been tested in South Africa.
This includes Prep (pre-exposure prevention), a medicine that stops the HIV-negative people to capture the virus.
Another breakthrough preventive drug, released this year, Lenacapavir, an injection taken twice a year and this offers complete HIV protection, has also been tested in South Africa.

At the Laboratory in the Campus for Health Sciences at the University of Whits, a small group of scientists still work on the HIV vaccine.
They are part of the brilliant consortium, a group of laboratories operating in eight African countries to develop a virus vaccine.
“We were developing a vaccine test to see how well it works and then we would try it on people,” says Abdula Eli, an associate professor at Whits University, tells the BBC in his lab.
“The plan was to conduct tests in Africa based on studies conducted by Africans, because we want this study to be beneficial for our community as well as all humanity.”
But the redundancies of US funding have called out their work.
“When the suspension order came, it meant that we needed to stop everything. Only some of us managed to receive additional funding so that we could continue our work. It was back for months, it may even be a year,” says Prof. Eli.
There is no funding in the laboratory for clinical trials scheduled for later this year.
“This is a very big loss for South Africa and the continent. This means that any potential study coming out of Africa will have to be tested in Europe or the United States,” says Prof. Eli.
In June, universities demanded the rescue government of 4.6 billion South African Rand ($ 260 million; 190 million British pounds) over the next three years to cover some of the US -lost funding.
“We are praying for support because South Africa is a leader in HIV’s research, but this is not a leader for itself. It has consequences of the practice and policies of the world,” says Dr. Fati Matu, the head of universities in South Africa.
South Africa Health Minister Aaron Motoes have announced on Wednesday that some alternative funding has been provided for research.
The Foundation Bill and Melinda Gates and Welcom Trust agreed to donate 100m Rand with immediate effect, while the government would provide 400m Rand over the next three years, he said.
This will lead to the total number of up to 600 M Rand, far less than 4.6 billion Rand, requested by researchers.
As for Gugou, she hoped that by the time she was adult, he would be found for HIV/AIDS treatment, but now it is less optimistic.
“I look for nine years old. I want to live as long as I can continue to take care of it,” she tells the BBC.
“This is not just a problem for now, we have to think how it will affect the next generation of women and young people.”
 Getty Images/BBC
Getty Images/BBC