Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
 Ghetto images
Ghetto imagesTen: This is the era of the richest man with HIV, who has once met.
When the Network for Intercession for Survivors from Fiji in 2013 began for the first time, this young boy is yet to be born. He is now one of the thousands of Fijians who has become infected with the blood virus in recent years – many of them at the age of 19 or the younger and many of them through intravenous drug use.
“More young people use drugs,” says G -Naitala, whose organization provides support for sexual workers and drug users in the Fiji capital SUVA, “BBC told the BBC. “He (the boy) was one of those young people who shared needles on the street during Covid.”
In the last five years, Fiji, a tiny nation in the South Pacific with a population of less than a million – has become one of the fastest growing HIV epidemics in the world.
In 2014, the country had less than 500 people living with HIV. By 2024, this number has grown to approximately 5900 – eleven times jump.
In the same year, Fiji registered 1583 new cases, a threefold increase in his usual five-year average. Of these, 41 are 15 or smaller, compared to only 11 in 2023.
 Ghetto images
Ghetto imagesSuch figures have encouraged the Minister of Health and Medical Services of the country to announce an epidemic from HIV in January. Last week, Assistant Health Minister Penions Ravunava warned Fiji to record more than 3,000 new HIV cases by the end of 2025.
“It’s a national crisis,” he said. “And it doesn’t slow down.”
The BBC talks to numerous experts, defenders and first -line workers about the reasons for such a meteoric rise in the number of cases. Several have indicated that as awareness of HIV is spreading and the stigma decreases, more people go forward and are tested.
At the same time, however, they also noted that countless more are invisible to official data-and that the real scale of the edition is probably much larger than even the records suggest.
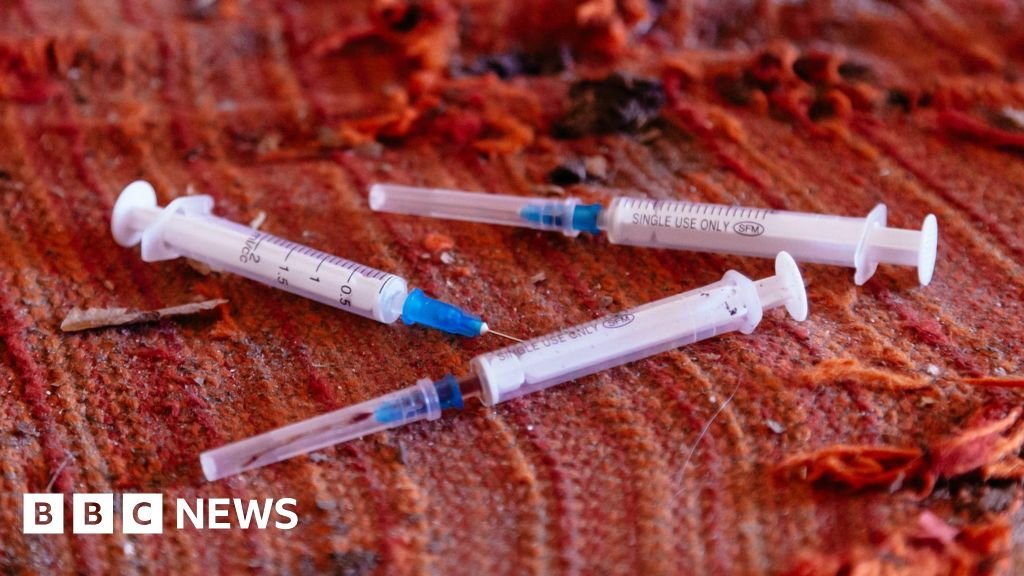
At the heart of the HIV epidemic of Fiji is a spiral trend for drug use, dangerous sex, needle sharing and “Bluetoothing”.
Otherwise known as the “hot spot”, this last term refers to a practice in which an intravenous drug user pulls his blood after shocks and injects it into a second person – who can then do the same for one third, etc.
Calesi Volatabu, CEO of NGO Free Free Fiji, saw that it was happening first -hand. Last May, she was on one of her regular walks from the early morning walks through the Fiji capital of Suva, offering support and education to drug users on the streets when she turned an angle and saw a group of seven or eight people together.
“I saw the needle with blood – it was right there in front of me,” she recalls. “This young woman, she had already fired and she removed the blood – and then you have other girls, other adults who are already arranged to be hit by this thing.
“It’s not just the needles they share – they share the blood.”
Bluetoothing is also reported in South Africa and Lesoto, two countries with some of the highest HIV rates in the world. In Fiji, the practice has become popular over the last few years, according to G -Ja Volatabu and D -Ja Naitala.
 Paid: Castle Volatabu
Paid: Castle VolatabuOne of the reasons for his appeal, they explain, is more cheaper: many people can find themselves for a hit and share it with each other. Another is the convenience of only needing one syringe.
They can be difficult to get Fiji where pharmacies, under pressure from the police, often require recipes for syringes and there are no needle programs.
Although the acceptance and approval of the deployment of such programs, which provide pure equipment to inject drug users in an attempt to reduce the transmission of blood infections such as HIV administration in a highly religious and conservative side, have been challenging.
Mrs. Volatabu says there is a “drastic shortage” of needle sites, which nourishes dangerous practices such as needle and Bluetoothing sharing and putting the weight of NGOs for syringe distribution as well as condoms.
In August 2024, the Ministry of Health and Medical Services of the Fiji (MOH) recognized Bluetoothing as one of the leaders of the country’s rise in the cases of HIV. Another was Chemsex, where people use medicines – often methamphetamine – before and during sexual meetings.
In Fiji, unlike most other countries around the world, crystal meth is consumed mainly by intravenous injection.
MOH also found that out of 1093 new cases, registered in the first nine months of 2024, 223 – about 20% – are from intravenous use of medicines.
Fiji has become the main hub for the Pacific Traffic for Crystal Met over the last 15 years. Much of this is due to the country’s geographical location between East Asia and America – some of the world’s largest drug producers – both Australia and New Zealand – the highest paid markets in the world.
During the same period, Met spilled and spread to local communities, developing in a crisis that, like HIV, was recently declared a “national emergency”.
According to those on the front lines, the age of the users tends to be down.
“We see more and more than these young people,” says G -Ja Volatabu. “They are becoming more young and younger.”
The most national HIV statistics of Fiji cites the use of injection injection as the most common known method of transmission, which represents 48% of cases. Sexual transmission represents 47% of cases, while the transmission from mother to child during pregnancy and childbirth is cited as the cause of most pediatric cases.
Everyone to whom the BBC talk has agreed that a lack of education is a central factor in the epidemic. D -Ja Volatabu and D -Ja Naitala work and change -and d -naitala says that as a greater awareness of the dangers of the spread of HIV throughout the community, Bluetoothing has been in favor in its experience.
More people are testing and looking for HIV treatment, leading to more stable data around the scale of the crisis.
But there is still concern that the official number of cases is just the tip of the iceberg – and the fear of what can be hidden below the surface.
Jose Susa-Santhos, head of the Pacific Regional Security Center at the University of New Zealand in Canterbury, says “has boiled a perfect storm.”
“The concern is at all levels of society and the government regarding the Fiji HIV crisis – not only what is happening at the moment, but also where it will be in three years and the lack of Fiji resources,” he told the BBC. “Maintenance systems – breastfeeding, ability to distribute or access to HIV treatment medicines – are just not there.
“It terrifies us, the people who work in the region: there is no way Fiji can handle it.”
 Delivered: Jose Susa-Santos
Delivered: Jose Susa-SantosFollowing its fire statement in January, the Fiji government tried to improve its HIV monitoring and improve its ability to cope with the likely non -grading cases.
The global warning and response network, which was called to provide this support, said in a recent report that “addressing these urgent problems through a well -coordinated national response is crucial to reversing the HIV epidemic in Fiji.”
This report also notes that the shortage of staff, communication problems, challenges with laboratory equipment and stocks of fast tests and HIV drugs affect screening, diagnosis and treatment.
Data collecting is slow, difficult and predisposed to errors-it prevents it-it prevents efforts to understand the degree of HIV epidemic of Fiji and the effectiveness of the reaction of the hearth.
This leaves many experts, authorities and daily Fijians in the dark. And Mr Sousa-Santos predicts an “avalanche” of cases that are yet to come.
“What we see right now is the beginning of the avalanche, but you can’t stop it because infections are already happening now or they have already happened – we just won’t be able to see them and people will not seek to be tested for two to three years,” he says.
“There is nothing to do right now to stop the number of infections that have already happened in the last year, and this is happening now. It’s really horrifying.”